Transcranial magnetic stimulation (TMS) is a non-invasive psychiatric treatment that does not require drugs and has little to no side effects. Since being approved by the FDA to treat major depressive disorder in 2008, TMS has quickly risen as an alternative treatment option for patients with treatment-resistant depression.
But because TMS is machine-operated, a technician must be present at every treatment session in order to ensure that the procedure is being carried out correctly.
Continue reading for more information regarding:
- TMS therapy, including how it works to create changes in the brain
- The job of a TMS technician, and how technicians are trained
TMS Therapy: An Overview
TMS uses magnetic pulses to stimulate brain cells. These pulses are channeled through an electromagnetic coil, which is placed against the patient’s head. TMS has many uses, both as a therapeutic tool and a piece of scientific equipment.
Therapeutic Tool
Right now, TMS is most commonly used to treat depression, though it was recently approved in 2018 to treat obsessive compulsive disorder (OCD) as well. In the past, studies have shown that depression is not merely an emotional phenomenon—it also affects the brain physically, causing it to function differently than a neurotypical brain.
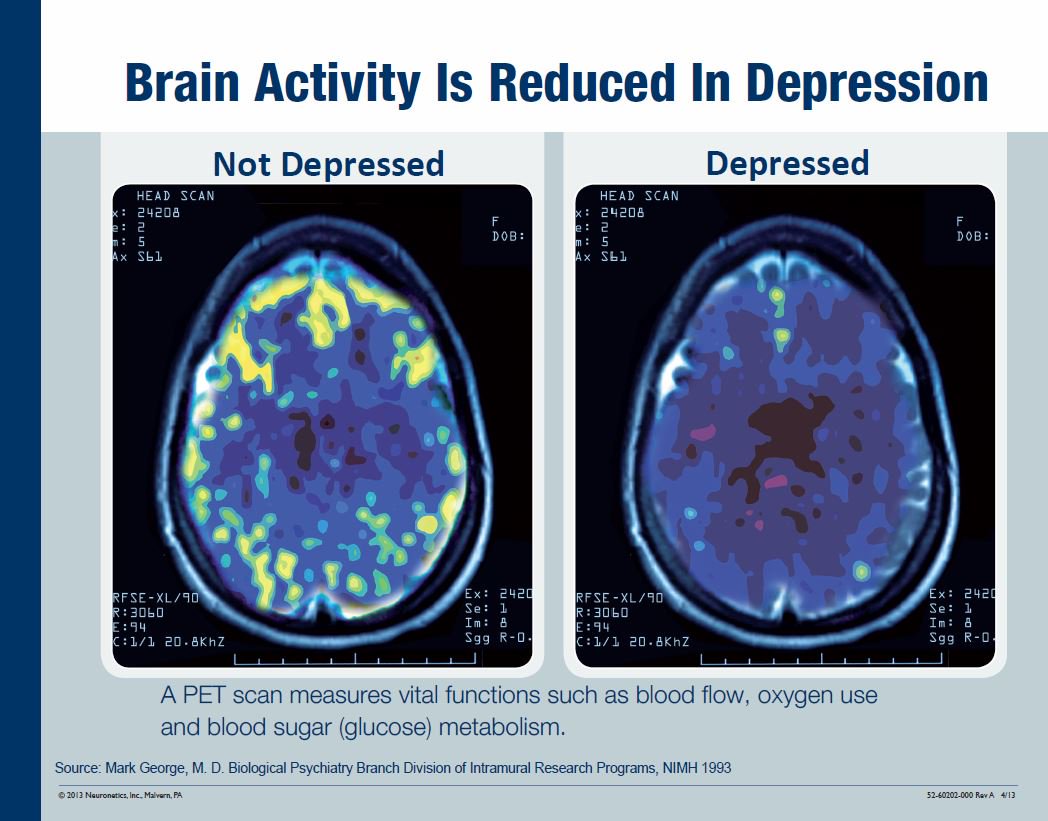
Depression can impede brain function and even cause certain areas of the brain to shrink. In addition to mood, memory and decision-making can also be negatively impacted by depression. TMS can help to reverse this damage—as well as other symptoms of depression—by interacting with the brain’s chemical makeup in order to create long-lasting structural changes.
Scientific Aid
Because TMS is non-invasive, safe, and tolerable, researchers have been able to use it as an aid in various scientific studies, specifically those concerning the brain and the nervous system. TMS allows researchers to stimulate targeted areas of the brain in order to learn more about the way it works, which can lead to better treatments for different conditions and diseases.
More Details about TMS Therapy
TMS is an outpatient therapy that is administered five days a week for around six weeks. The length of the sessions is specific to each patient, though thirty to forty minutes is the average timeframe.
While the treatment is relatively painless, the patient’s body usually requires some time to adjust to the magnetic pulses. This means patients might get headaches or irritation around the treatment site during or after sessions.
In order to achieve maximum accuracy, patients must remain still for the entirety of each session, though they are seated comfortably with head and neck support. TMS does not have any effect on cognition, so patients can resume their regular schedule following each treatment.
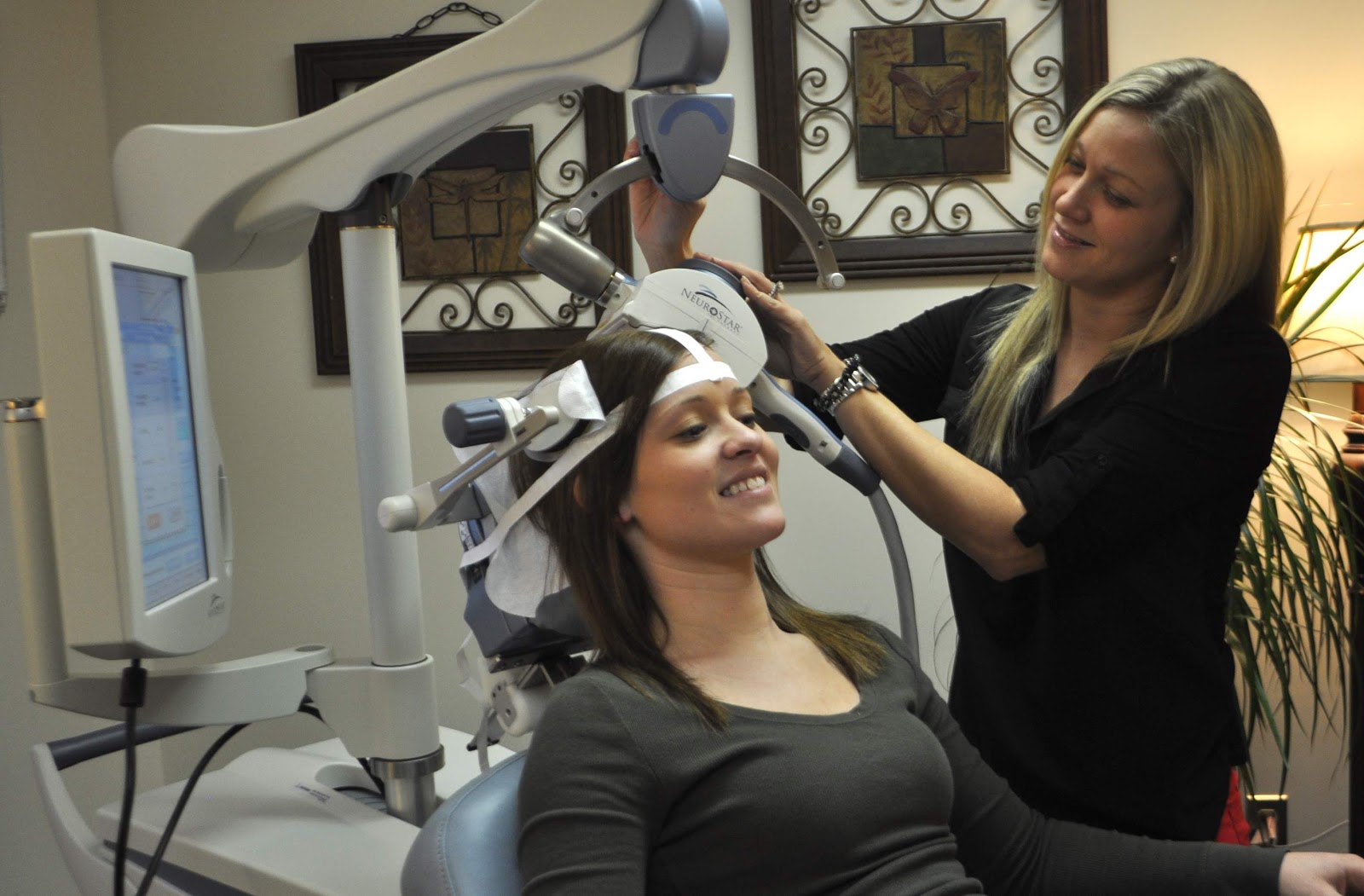
During a TMS session, the patient can watch TV or listen to music. A technician oversees the treatments, so basically all the patient has to do is sit still. Image courtesy of Guidance Center.
TMS is covered by most insurances for patients with major depressive disorder who have tried at least one antidepressant and psychotherapy. Because TMS uses a magnet, patients with non-removable metalware near or around the head might not be approved for treatment.
TMS Technicians
Who Are They?
TMS technicians usually have a background in medicine or psychology, and prior experience working with patients in a medical office or mental health facility is a common prerequisite. Before becoming a certified TMS technician, applicants must undergo training, typically in the form of a short course that includes traditional study as well as hands-on guidance. Sometimes, this training can be done partially online.
Because TMS technicians interact with patients all day, every day, interpersonal communication skills are a necessity. An aptitude for administrative work is also a valuable trait to have as a technician, along with the capacity to learn to work medical equipment.
What Do They Do?
Though patients will meet with a psychiatrist before starting treatment, the TMS technician is the one present during the actual sessions. In addition to operating the TMS machine, the technician also records the patient’s progress and conducts regular check-ins to monitor any physical or emotional changes, such as weight loss or change in sleep.
Interested in TMS? Learn More Today
As many as 40 percent of patients don’t respond to antidepressants. Has your depression persisted despite medication and therapy? TMS could be right for you. Talk to your doctor, and find a TMS provider near you today.
